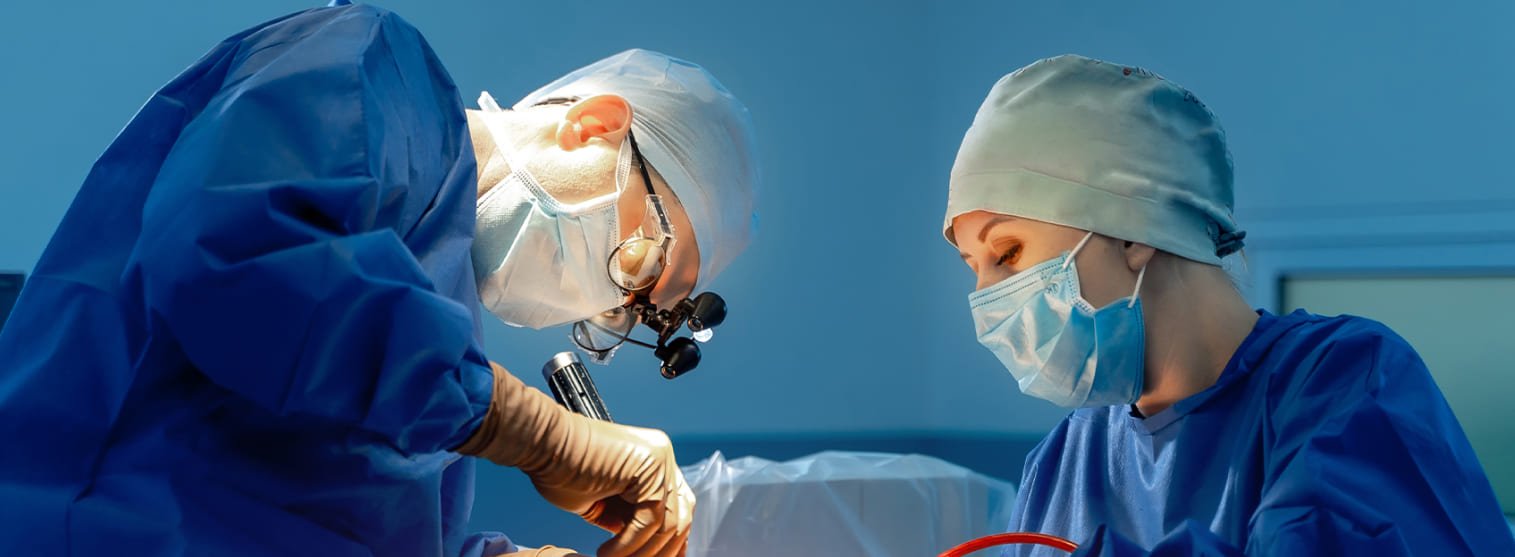
Life in the Operating Room
Operating rooms are always mysterious places for outsiders, and frightening for most people. No one except the staff comes to the operating rooms cheerfully. However, for surgeons, anesthesiologists, anesthesiology technicians and technologists, operating room nurses, and auxiliary healthcare personnel working in the operating room, they are not difficult places at all. Work is usually organized according to a predetermined schedule. Many questions have already been answered in advance, such as which patient will undergo surgery and at what time, which doctor will operate on which patient and when, which anesthesiologist will administer what type of anesthesia to which patient, and whether the patient will be transferred to the ward or intensive care after surgery. To ensure this order is maintained, patients scheduled for surgery must be evaluated by an anesthesiologist at the anesthesia clinic at least 24 hours in advance. Necessary preoperative tests must be performed to avoid surprises, opinions from other specialists must be sought if needed, patients or their relatives must be informed about the anesthesia methods to be used and their consent must be obtained, and it is very important to ensure that patients fast for at least 6-8 hours before surgery. Of course, there are also some unexpected developments that cannot be ruled out. Examples include a patient who is urgently scheduled for surgery being rushed into the operating room, the availability or unavailability of a suitable operating room at that moment, unexpected bleeding during surgery, organ damage, and other undesirable events.
What is the physical structure of the operating rooms?
The operating room entrance must have a single door and the access to it should be controlled. The number of operating rooms should be adjusted according to the number of beds in the surgical clinics (one room for every 25-30 beds). There should be three different areas in the operating room (sterile area, clean area, non-clean area). The sterile area consists of operating rooms and rooms where sterile instruments are prepared. The clean area consists of corridors leading to operating rooms, rooms where preoperative and postoperative patient monitoring is performed, rest rooms, and sterile storage rooms. The non-clean areas consist of patient waiting rooms, recovery rooms, and washrooms. These areas must be completely separated from each other. Staff movement between these areas must be controlled. Rooms where sterile materials are stored must be clean, and these materials must be kept in closed cabinets. Sterile materials and used materials must not be stored in the same environment. Closed carts must be used to transport sterile materials to the operating room.
What medical devices are found in an operating room?
Although the medical devices used in operating rooms vary depending on the surgeries performed at that hospital, some medical devices are essential for operating rooms. These include, in order: Operating Table, Operating Room Ceiling Light, Surgical Aspirator, Anesthesia Machine, Patient Monitoring Device, Defibrillator, Electrocautery, and Infusion Pump. Stainless Steel Hospital Equipment and Surgical Hand Instruments found in operating rooms are also auxiliary equipment that complete operating rooms and are of considerable importance.